The changes in the inspection regime by the Care Quality Commission...
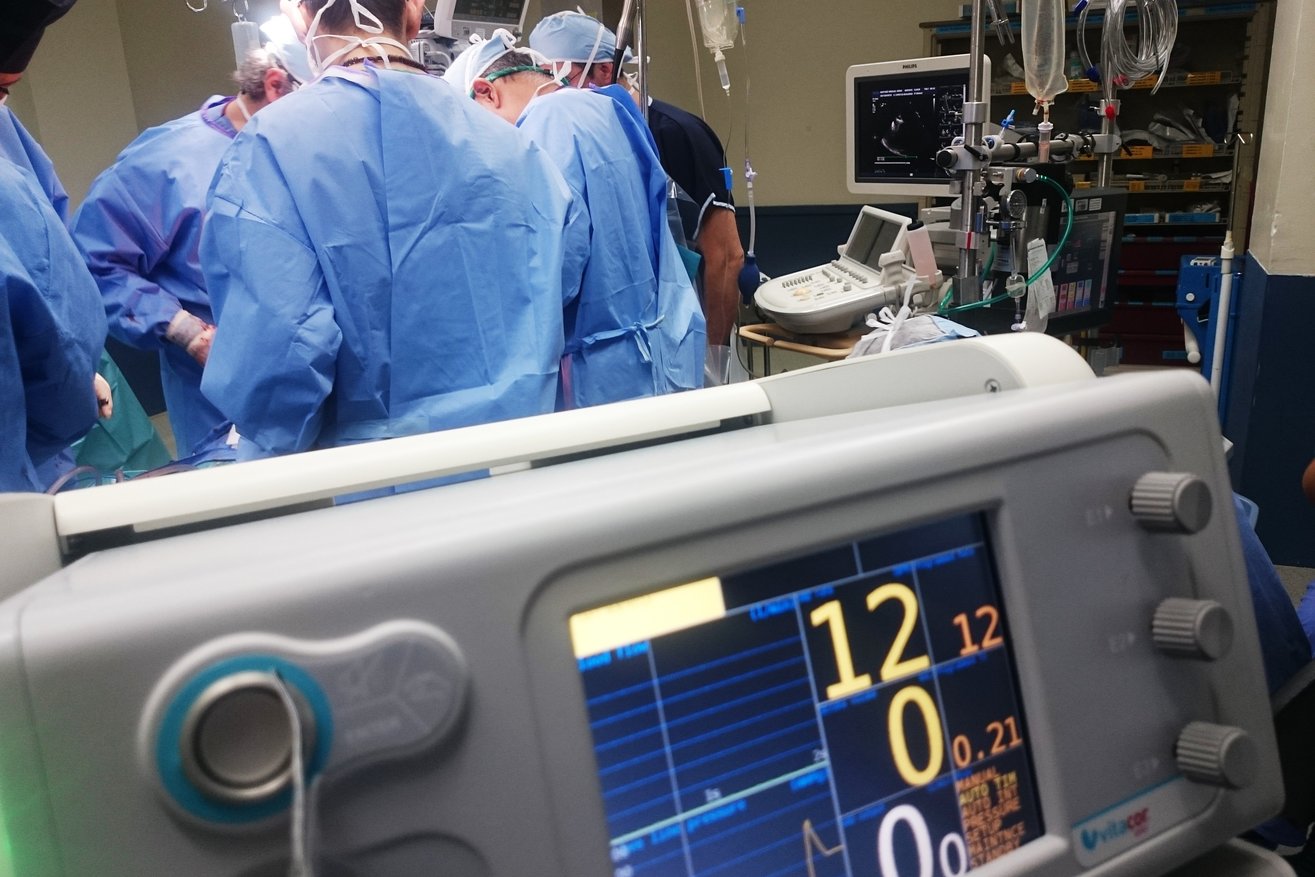
It has been over two years since I assumed the running of the Interim Healthcare Practice and in that time the sector has been through unparalleled levels of evolution; some changes have been for the better whilst others have certainly divided opinion.
From our point of view, it has been a tremendous 28 months with many successful interim placements across the whole of the UK, which include Chief Executive Officer, Director of Nursing , Director of Finance, Chief Operating Officer, Governance leads and Turnaround Directors as well as Transformation roles. We have also made significant inroads into new areas having successfully built traction within the Private Healthcare and Care Home industries.
Like the NHS, these private industries feel the effects of Government spending cuts and increasing regulatory scrutiny, with the added pressure of needing to at least break even in order to stay in business. The Private Hospital sector is entering a significant period of change, as a Competition Commission ruling looks set to result in two firms having to sell hospitals, as well as the upcoming sale of at least one of the industry’s biggest operators.
However, the real purpose of this piece is to look at the main trend that is really driving the Healthcare sector at present. It is a hard one but – after much deliberation – I decided the most topical and high profile angle had to be the changes in the inspection regime by the Care Quality Commission (CQC) following the Francis, Keogh and Berwick reports as a consequence of Mid Staffordshire and other high profile care failures.
As many of you will know, Professor Sir Mike Richards has now been in his new role as the first Chief Inspector of Hospitals for several months. He has certainly made an impact and, working alongside a strong team of specialist inspectors, he has been asking all of the services he inspects the same question: “Are you safe, effective, caring, responsive to people’s needs and well led?”
Sir Mike was the keynote speaker at our annual Healthcare Dinner a couple of months ago. His insight made for fascinating listening, as he gave the assembled audience an overview of the challenges in developing consistent processes and assembling strong teams to assess performance and quality across all services of a Trust, judging them across five separate criteria asking the question above, before being issued one of four possible quality ratings: “Outstanding, Good, Requires Improvement or Inadequate”. Ultimately, each inspection will provide the public with a clear picture of the quality of care in their local hospital.
The central issue is most certainly around obtaining an accurate picture of quality as well as the willingness of every Trust’s leadership team to be transparent about the issues which need to be scrutinised. This needs to happen from the very beginning and before an inspection can even begin.
It has been interesting to see that some Trusts have been achieving outstanding results in certain services, only for another of their services to fail an inspection. As with any large scale change, this has resulted in a great deal of political and media commentary, as well as drawing both praise and criticism from some of the NHS’ most senior figures. However, there is no doubt that it is good to have a broader and more transparent understanding of the quality of care on offer within any given Trust.
Since the inspection regime was rolled out in the Autumn of last year, we have seen a notable rise in the demand for high impact interims - specifically for those who are able to add value covering the whole range of responsibilities. Forward thinking Trusts see the inspection regime as a safety net, recognising the need to assure themselves of their performance in advance of external scrutiny. One of the biggest requirements has been the need for quality, risk and clinical governance executives who can assess the services concerned and make and/or implement recommendations to ensure that Trusts are running their services in line with the Regulators expectations.
Despite these turbulent and unpredictable times, I’m happy to report that feedback from our clients has been overwhelmingly positive – interim executives quickly add significant value over a short period of time to ensure that any given Trust is able to make progress.
To sum up, the future of the Healthcare sector is going to be determined and shaped by the talents and skills of its leadership teams. In my view, interims have shaped - and are shaping - a new way of thinking but fundamentally, existing and future leaders will need to be champions of innovation and new thinking, which is no means an easy task when faced with continual financial challenges, staff turnover and efficiency drives.